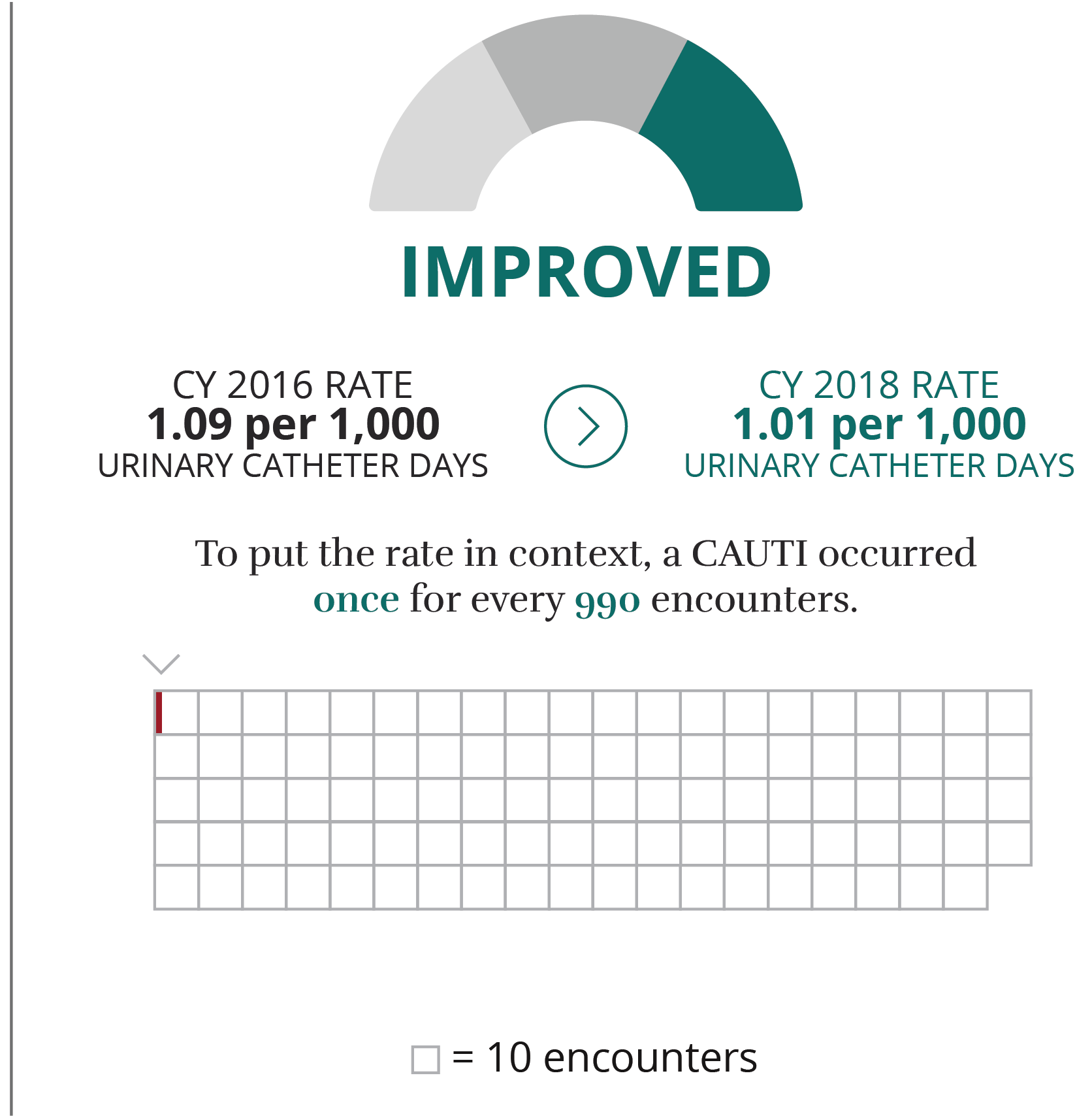
What is it?
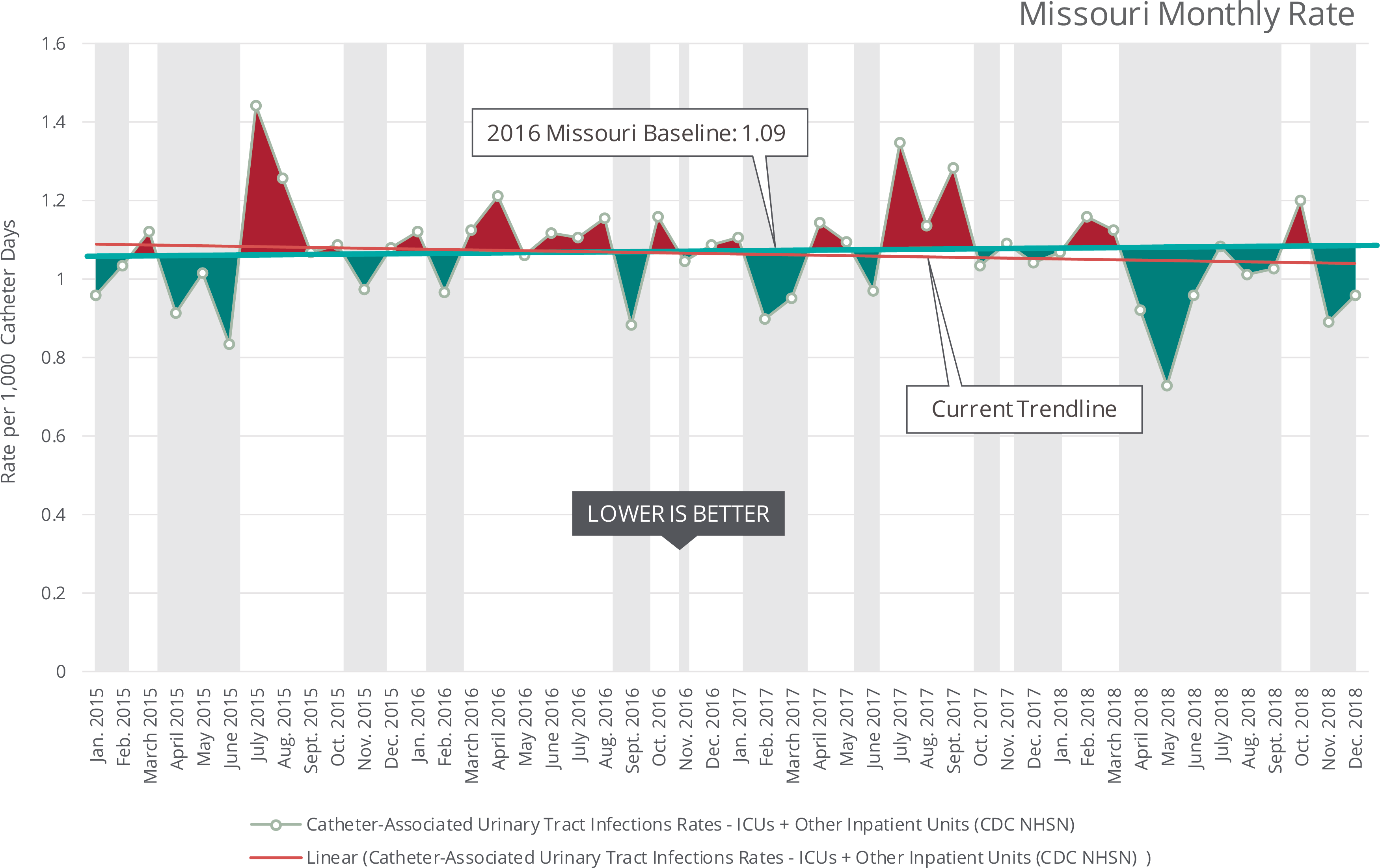
A urinary tract infection is an infection that involves any part of the urinary system, including urethra, bladder, ureters and kidney. Among UTIs acquired in the hospital, approximately 75 percent are associated with a urinary catheter, which is a tube inserted into the bladder through the urethra to drain urine. Between 15 and 25 percent of patients receive urinary catheters during an inpatient stay. The most common and most important risk factor for developing a catheter-associated UTI is prolonged use. Therefore, catheters only should be used for appropriate indications and removed as soon as they are no longer medically needed.
How’s it measured?
The rate is per 1,000 urinary catheter days. Urinary catheter days are calculated by dividing the number of CAUTIs by the number of catheter days and multiplying the result by 1,000.











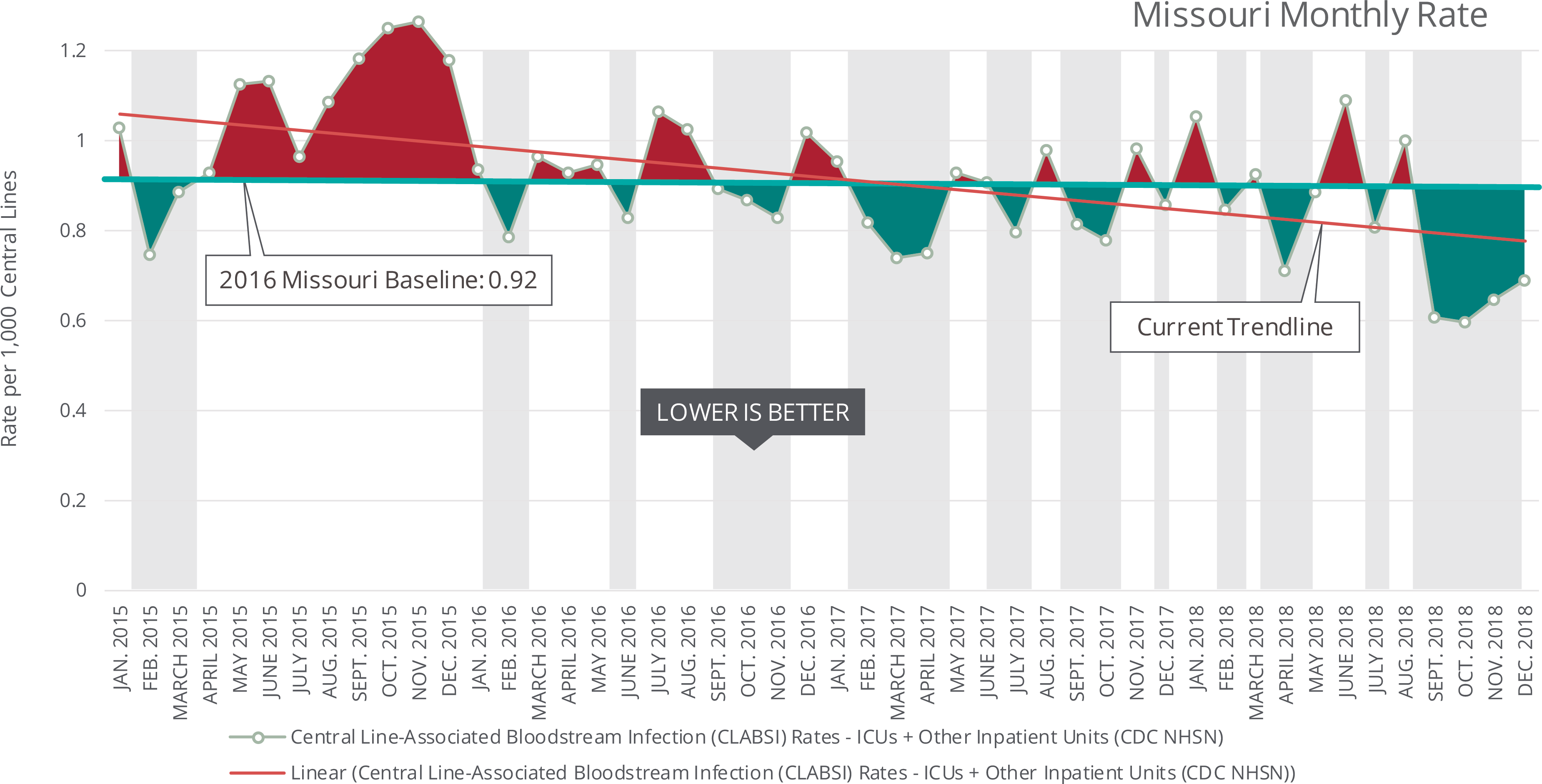
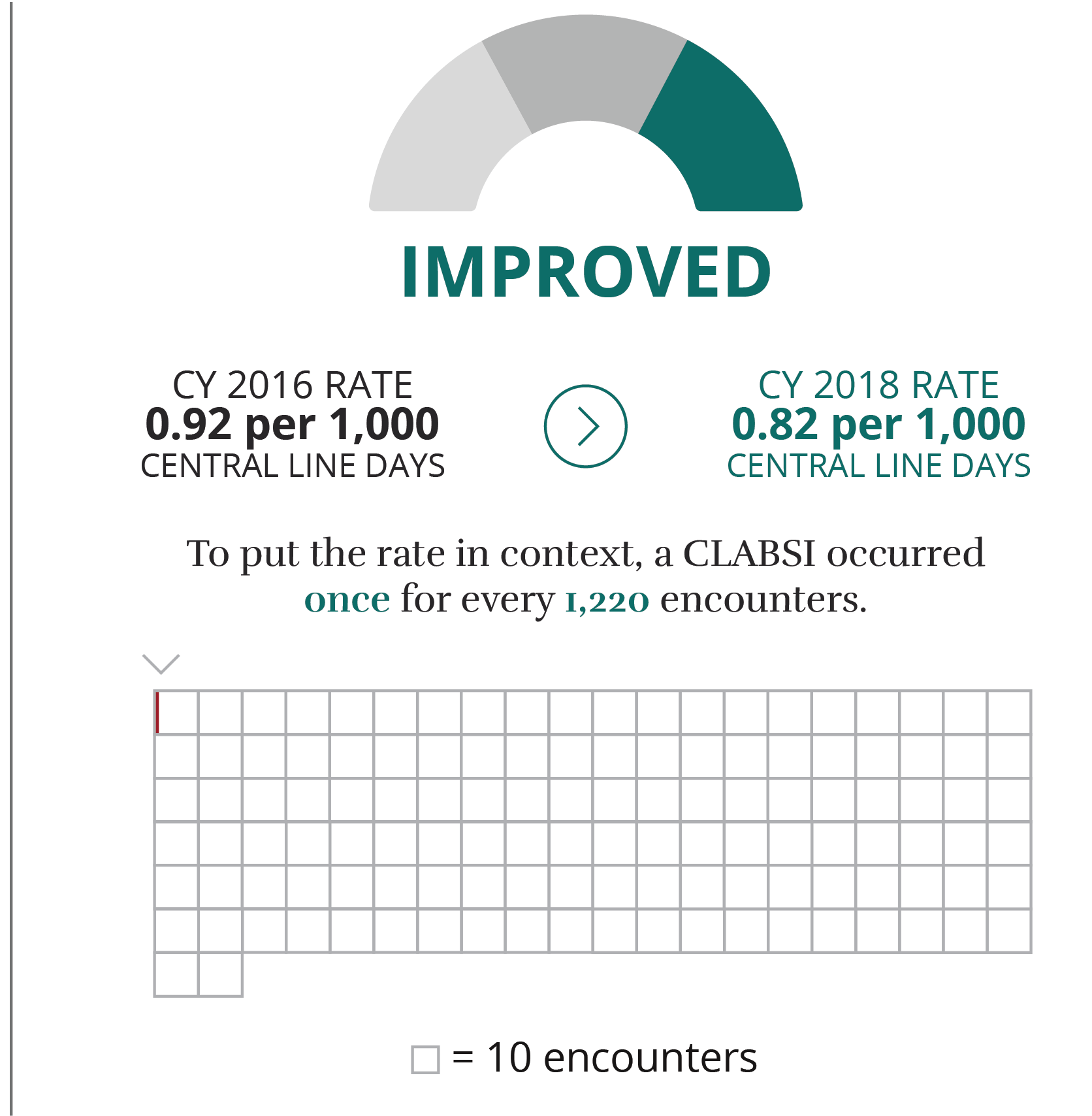

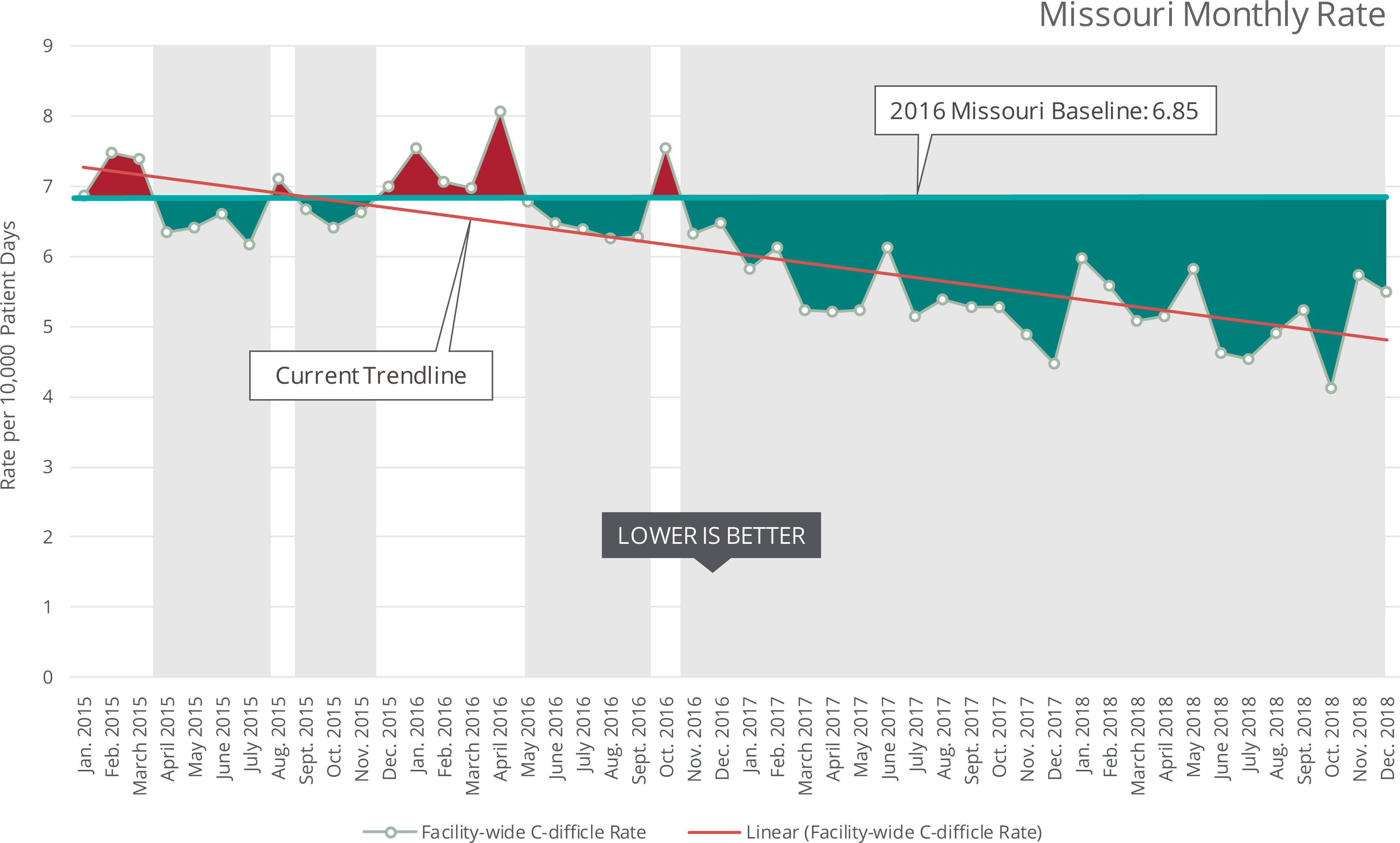
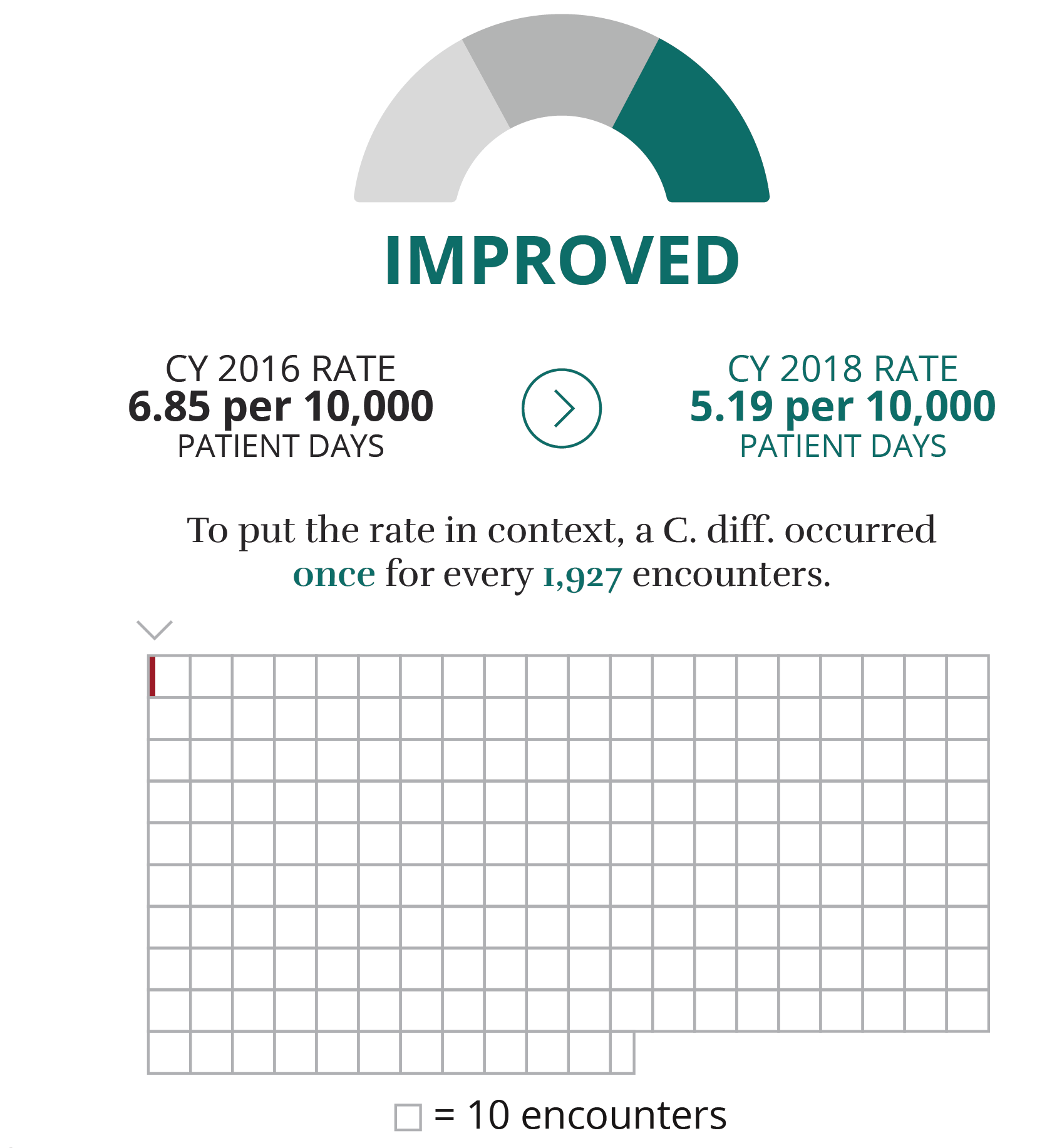 What is it?
What is it?
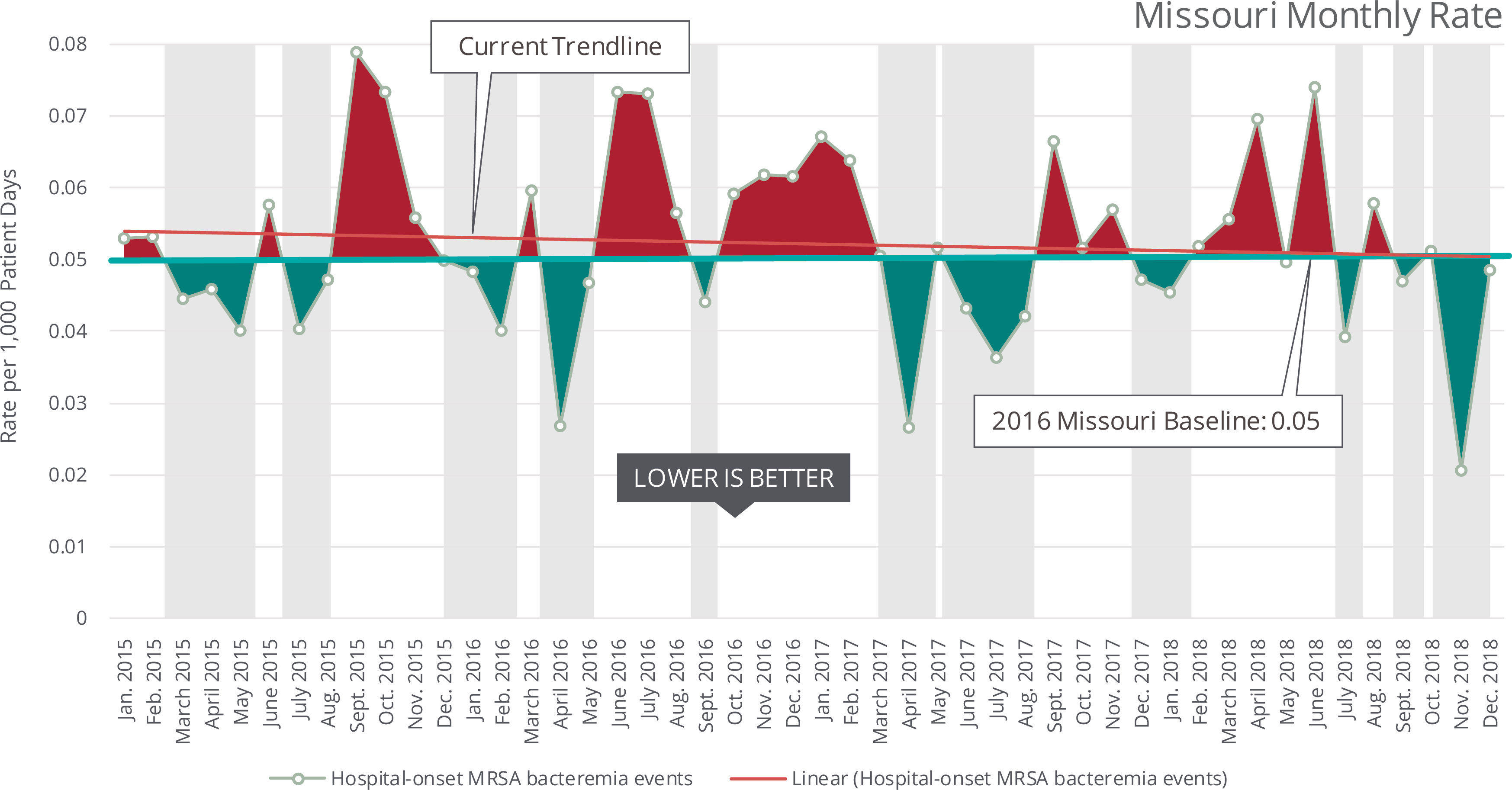
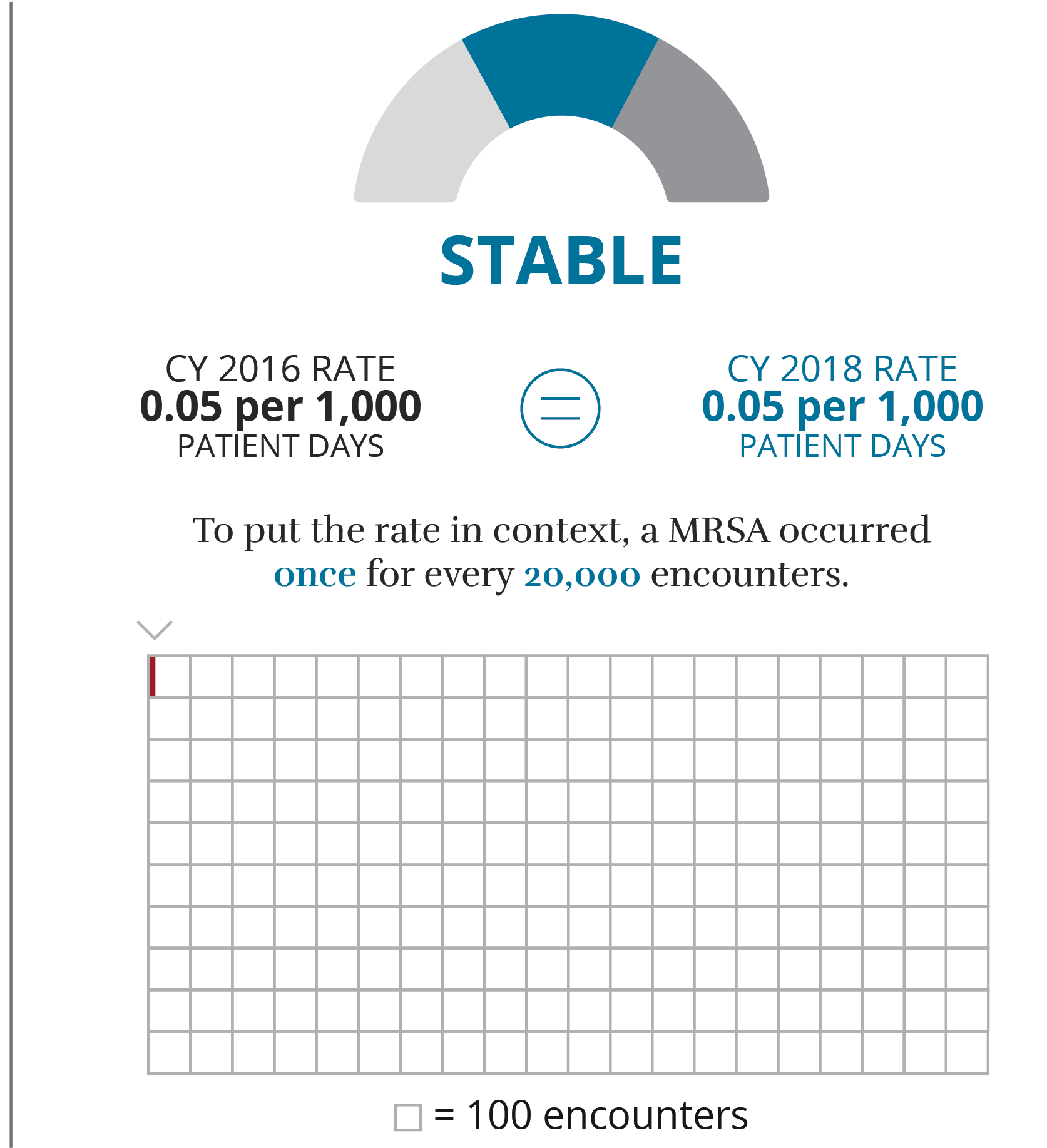 What is it?
What is it?
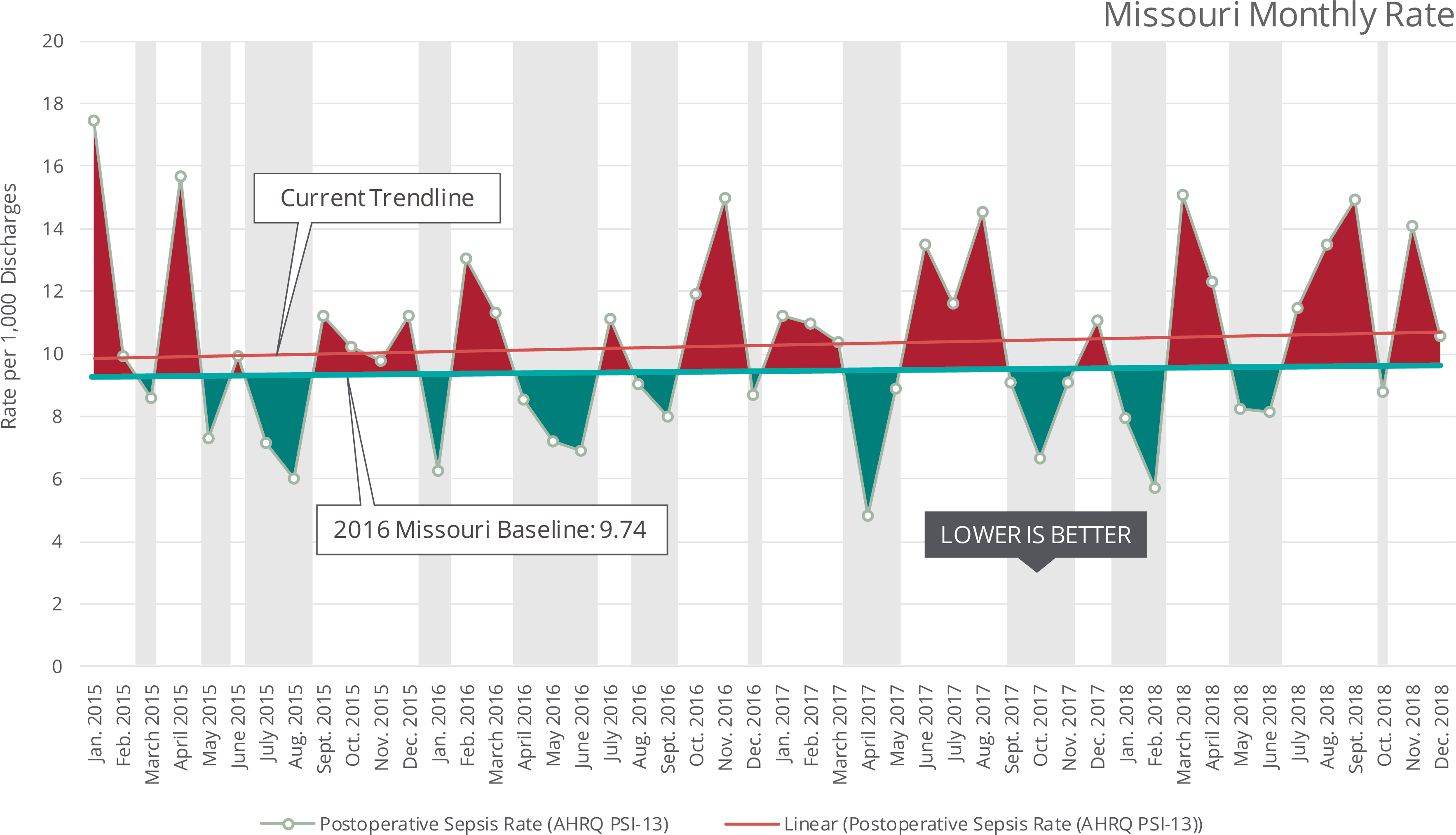
 What is it?
What is it?