Staff Contact: Andrew Wheeler
MHA released a summary and analysis of the federal fiscal year 2021 Inpatient Prospective Payment System final payment and policy updates. The analysis includes the financial effects of market basket updates, the budget neutrality adjustment, reductions mandated by the Affordable Care Act, Medicare disproportionate share changes, quality-based payment adjustments and coding adjustments. Results are illustrated in national, Missouri, health system and individual hospital groupings. IPPS hospitals in Missouri are projected to receive an estimated 1.7% increase in Medicare payments. Although footnoted, the effects of the Medicare sequestration are not included.
Policy and analytic studies, prepared for distribution by the Hospital Industry Data Institute, are available for download to authorized users of HIDI Analytic Advantage®.











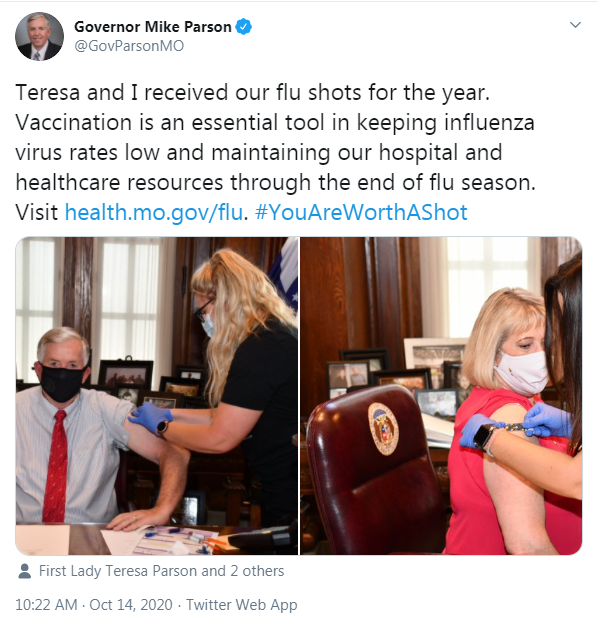 In other years, some patients approach the flu vaccine with a healthy dollop of skepticism. After all, there often are side discussions of whether any year’s vaccine is well matched, if the vaccine is worth the trouble of arranging for a provider to administer it and whether protection matters if you aren’t in an at-risk population. This year, the stakes are very different.
In other years, some patients approach the flu vaccine with a healthy dollop of skepticism. After all, there often are side discussions of whether any year’s vaccine is well matched, if the vaccine is worth the trouble of arranging for a provider to administer it and whether protection matters if you aren’t in an at-risk population. This year, the stakes are very different.